2 results
Psychological Inflexibility in Depression with Psychotic Features: A Case Report
- S. Akyildirim Cor, S. Yetkin
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1027
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Major depressive disorder (MDD) is a mood disorder that can last for weeks or even months, in which there is a depressed mood accompanied by anxiety, in addition to negative changes in cognitive functions, psychomotor movement and vegetative functions. Depression with psychotic features is a psychiatric syndrome that progresses with delusions as well as severe symptoms such as psychomotor retardation or agitation, depressive ruminations, deterioration in cognitive functions, and confusion. Compared to the subtypes without psychotic features, the symptoms are more severe, the age of onset is earlier, and the duration of the disease is longer. Feelings of guilt, worthlessness and suicidal thoughts and attempts at suicide are more common. The risk of exacerbation is greater. Diagnosis of bipolar disorder and schizophrenia is more common in first-degree relatives of these patients.
ObjectivesAn 18-year-old female patient with somatic delusions and psychotic persistence that started after a sexual trauma and persisted for 1 month was consulted after organic exclusions were made. It is understood from the anamnesis that the patient had a manic episode about 6 months ago and that his mother was followed up with a diagnosis of bipolar disorder. The patient’s current clinical picture was evaluated as depression with psychotic features, and after hospitalization, the treatment was adjusted as fluoxetine 20 mg/g, olanzapine 5 mg/g, and lithium 900 mg/g. Self as context, cognitive defusion and acceptance interventions were applied to the patient.
MethodsWhen the Cognitive Fusion Questionnaire(CFQ), Self-as-Context Scale(SACS), Acceptance and Action Questionnaire(AAQ-II) completed by the patient during hospitalization and in remission periods were compared, it was observed that there was a significant regression in the patient’s psychological inflexibility during the period of remission. Written informed consent was obtained from the patient whose clinical picture was presented in order to contribute to the scientific literature.
ResultsDepression with psychotic features is another clinical picture in which psychological inflexibility increases, and it has been observed that interviews to increase psychological flexibility during the treatment process contribute positively to the treatment process. For this reason, the contribution to the healing process can be better clarified in further studies on interventions to increase psychological flexibility applied in addition to pharmacological treatments.
Image:
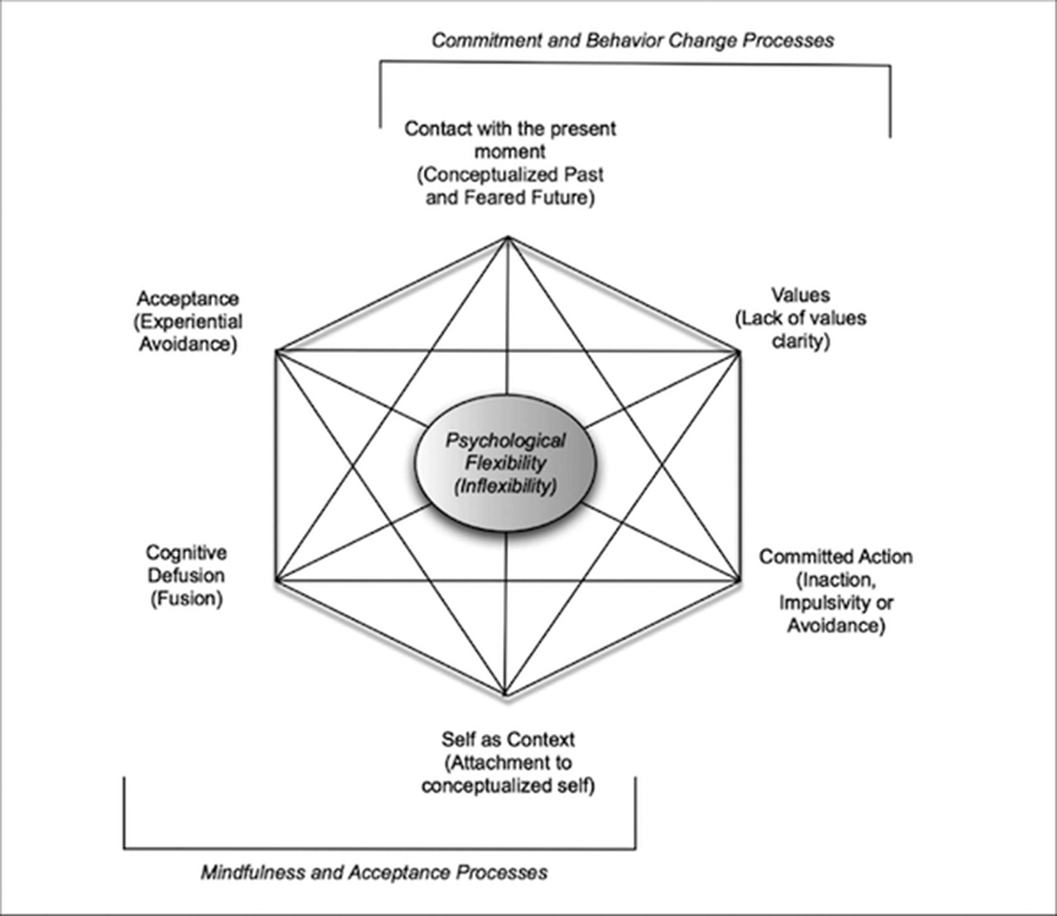 Conclusions
ConclusionsPsychological inflexibility is an effort to control a person’s emotion, thought, behavior or experience in a dysfunctional way in the face of an undesired experience. It has been seen in studies conducted in recent years that; There is a significant positive correlation between high psychological inflexibility and somatization, depression, anxiety and other psychological disorders.
Disclosure of InterestNone Declared
P-961 - Changes in the Sleep Structure of the Patients Diagnosed With Post-traumatic Stress Disorder
- B. Akcay, F. Ozgen, S. Yetkin, N. Lapsekili
-
- Journal:
- European Psychiatry / Volume 27 / Issue S1 / 2012
- Published online by Cambridge University Press:
- 15 April 2020, p. 1
-
- Article
-
- You have access Access
- Export citation
-
Introduction
Sleep disturbance is a common complaint among patients diagnosed with post-traumatic stres disorder (PTSD). Polysomnography is one of objective methods used to better understand the pathophysiology of PTSD. But consistent results of polysomnography have not been obtained so far.
ObjectiveThe aim of this study is to investigate sleep structure and the relationship between sleep variables and clinical symptoms in adult male PTSD patients with combat trauma, with or without comorbid psychiatric disorder and without any medication.
Methodology30 PTSD patients and 19 healthy subjects exhibit similar characteristics in terms of age and sex were included in the study. Two consecutive overnight polysomnographic sleep study were performed to investigate sleep patterns.
ResultsIn this study we found that compared with normal controls, PTSD patients exhibited difficulty in starting sleep, reduced sleep efficiency, decreased total sleep time, prolonged sleep latency, increased Stage-1 sleep, increased REM density and REM sleep, increased phasic EMG activity percentage. Also, comorbid psychiatric disorders accompanying PTSD affected the structure of sleep and there was a significant relationships between symptom severity and sleep variables.
ConclusionAlthouh the relationship between symptom severity and sleep parameters was found significant, there was no relationship between the changes of sleep parameters and shape of the traumatic event, elapsed time after injury and deterioration in the integrity of the body. In the PTSD patients we observed disturbed sleep patterns (Sleep continuity, sleep structure, REM sleep) which support the finding that these patients are in an arousal state even at night.




